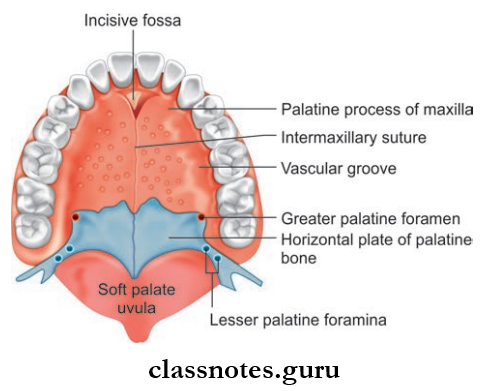
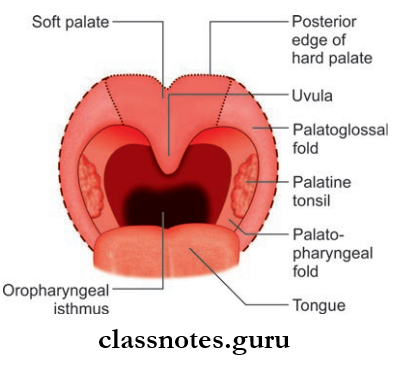
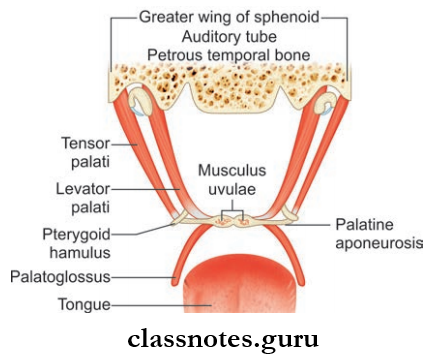
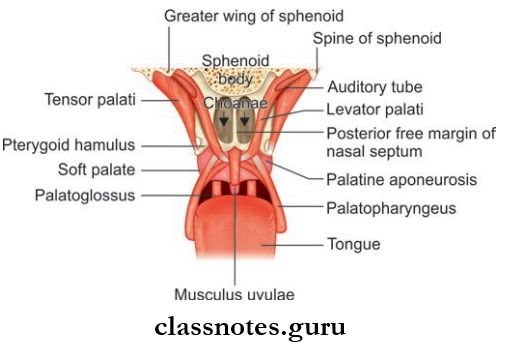
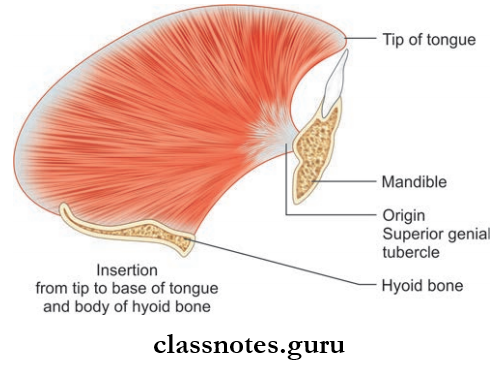
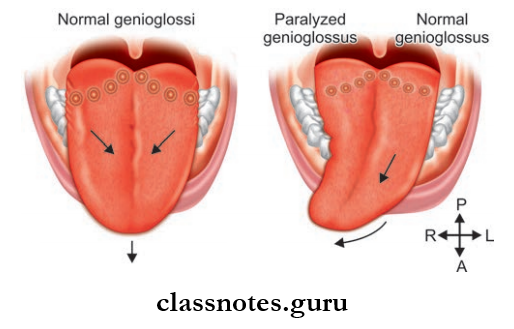
Surface Landmarks And Features Introduction
Forehead: Part of the face between hairline of the adolescent scalp and eyebrows.
Frontal Eminence: Superolateral prominence of the forehead.
Dorsum Of The Nose: Prominent ridge separating right and left halves of the nose.
Root Of Nose: The upper narrow end of nose just below forehead.
Columella: The soft median partition that separates two nostrils.
Palpebral Fissure: An elliptical opening between two eyelids.
Canthi: The lateral and medial angles of the eye.
Oral Fissure: The opening between upper and lower lips.
Philtrum: Median vertical groove on the upper lip.
Auricle/pinna: The superficial projecting part of the external ear.
Supraorbital Margin: Lies beneath the upper margin of the eyebrow.
Supraorbital Notch: Palpable at the junction of medial one-third and lateral two thirds of supraorbital margin.
Glabella: Median elevation connecting the superciliary arches and corresponding to an elevation between two eyebrows.
Scalp Temple And Face Question And Answers
Question 1. Describe the layers of the scalp.
Answer:
The Layers Of The Scalp


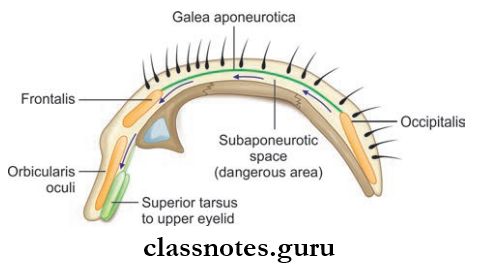
Layers Of The Scalp: Scalp refers to the soft tissues covering the cranial vault.
Layers Of Scalp Extent:
- Anteriorly: Up to the eyebrows
- Posteriorly: Up to superior nuchal line and external occipital protuberance
- Laterally: Superior temporal lines.
Layers Of Scalp Layers: Consist of 5 layers (from outside to inside)
- Skin: Thick and hairy, contain sebaceous glands and sweat glands, and is adherent to epicranial aponeurosis.
- Superficial Fascia: Fibrous and dense in the center than in the periphery. Binds skin to the aponeurosis vessels and nerves are present in this layer.
- The Third Layer Formed By:
- Mainly the epicranial aponeurosis (Galea aponeurotic)—the aponeurosis of occipitofrontalis muscle
- Occipitofrontalis Muscle Consisting Of:
- Occipital bellies arising from superior nuchal line
- Frontal bellies arising from the skin of the forehead
- Supplied by branches of the facial nerve.
- Fourth Layer Made Of Loose Areolar Tissue Which Extends
- Anteriorly into eyelids
- Posteriorly up to superior nuchal line
- Laterally to superior temporal lines.
- Emissary veins from the scalp to the sinuses traverse through this layer.
- Fifth Layer: Pericranium, which is loosely attached to the surface of bones, and at the sutures, the sutural ligaments bind it firmly to the endocranium.
- The first three layers are fully united to one another and they move together over the fourth layer.
Layers Of Scalp Applied
- Scalp bleed profusely due to rich blood supply.
- Loose areolar tissue layer is also known as a dangerous area of scalp because emissary veins that open here may transmit infection from the scalp to cranial venous sinuses.
- Avulsed portions of the scalp can be stitched back into position and heal well due to adequate blood supply even through the narrow areas of attachment.
- Due to the abundance of sebaceous glands, sebaceous cysts are common in the scalp.
- Bleeding in the scalp can be arrested by applying direct pressure over the wound against the bone.
- Bleeding in layer of loose areolar tissue forms a generalized swelling or spread widely reaching nuchal line posteriorly or temporal lines laterally, or can reach orbital margin and eyelids causing black eye.
- Cephalohematoma refers to the subperiosteal collection of blood bound by suture lines and assumes the shape ofrelated bones because periosteum loosely covers the bones except at the suture lines.
- Caput succedaneum is a subcutaneous edema occurring over the presenting part of the fetal head at delivery. It occurs due to interference of venous return during passage through the birth canal.
Mnemonics: SCALP
From Superficial To Deep:
- Skin
- Connective tissue
- Aponeurosis
- Loose areolar tissue
- Pericranium
Question 2. Describe the blood supply of the scalp and superficial temporal region.
Answer:
The Blood Supply Of The Scalp

- Arterial Supply
- The scalp on each side of the midline is supplied by five arteries, three in front of the auricle and two behind the auricle.
- These arteries enter from the periphery and freely anastomose with arteries of same side and cross anastomose with the other side.
- The scalp is a potential site of collateral circulation between internal and external carotid arteries.
- In front Of The Auricle
- Internal carotid artery → Ophthalmic artery → Supratrochlear artery → Supraorbital artery → External carotid artery → Superficial temporal artery
- Behind The Auricle
- External carotid artery → Posterior auricular artery → Occipital arteries
- Venous Drainage
- The scalp on each side of the midline is drained by fine veins and these accompany the arteries and have similar names.
- These Include: Supratrochlear and supraorbital veins unite to form an angular vein at medial angle of eye and continue as facial vein.
- The superficial temporal vein and maxillary vein unite to form the retromandibular vein and its anterior division in turn joins with the facial vein to form common facial vein.
- The posterior division of the retromandibular vein unites with the posterior auricular vein to form the external jugular vein which drains into the subclavian vein.
- The occipital veins drain into the suboccipital venous plexus.
- Emissary veins connect extracranial veins with intracranial venous sinuses.
- The diploic veins like the frontal diploic vein open into a supraorbital vein, the anterior temporal diploic vein drains to the anterior deep temporal vein, the posterior temporal diploic vein drains to the transverse sinus, and the occipital diploic vein drains to either occipital vein or the transverse sinus.

Question 3. Describe the nerve supply of the scalp and superficial temporal region.
Answer:
The Nerve Supply Of The Scalp

The scalp and the temple is supplied by ten nerves on each side. Out of this 4 are sensory and 1 is motor and 5 enter in front of the auricle and 5 enter behind the auricle.

Mnemonic: GLASSZ
- Greater occipital/Greater auricular
- Lesser occipital
- Auriculotemporal
- Supratrochlear
- Supraorbital
- Zygomaticotemporal




Since derived from the mesoderm of 2nd branchial arch they are supplied by the facial nerve
Topographically, Muscles Are Grouped Into Six Headings:
- Muscles Of Scalp
- Occipito frontalis
- Muscles Of Auricle
- Auricularis anterior
- Auricularia superior
- Auricularis posterior
- Muscles Of Eyelid
- Orbicularis oculi
- Corrugator supercilii
- Levator palpebrae superioris
- Muscles Of Nose
- Procerus
- Compressor naris
- Dilator naris
- Depressor septi
- Muscles Of Neck
- Platysma
- Muscles Around Mouth
- Orbicularis oris
- Levator anguli oris
- Depressor anguli oris
- Zygomaticus major
- Zygomaticus minor
- Levator labii superioris
- Depressor labii inferioris
- Levator labii superioris alaeque nasi
- Mentalis
- Risorius
- Buccinator
Main Muscles And Their Attachments

Superficial Temporal Region Applied: The involuntary part (smooth part) of the levator palpebrae superioris or Muller’s muscle is supplied by fibers from superior cervical ganglion and the paralysis of this muscle leads to partial ptosis in Horner’s syndrome.
Question 5. Describe the nerve supply of face.
Answer:
The Nerve Supply Of Face


Nerve Supply Of Face Applied
- In case of supranuclear lesions of the facial nerve associated with hemiplegia usually the lower part of the opposite side of face is paralyzed.
- Bell’s palsy: It is the lower motor neuron paralysis of facial muscles due to compression of facial nerve in the facial canal. Here the whole of the face of the same side gets paralysed. As a result, wrinkles are absent on the forehead, the inability to close eye is present, deviation of angle of the mouth to the normal side, and food accumulates between the cheek and teeth.
Question 6. Describe the venous drainage of face.
Answer:
The Venous Drainage Of Face


- The veins accompany arteries of the face and drain into a common facial vein and retromandibular vein and they communicate with cavernous sinus
- The vein on each side form a ‘W’ shaped arrangement and each corner of ‘W’ is prolonged upwards to the scalp and downwards to the neck
- The deep connections include:
- Communication between supraorbital and superior ophthalmic veins
- Communication with pterygoid plexus through deep facial vein.
Venous Drainage Of Face

Venous Drainage Of Face Applied
- Since, the facial vein communicates with the cavernous sinus, retrograde infection from face is possible and result in thrombosis of cavernous sinus.
- Mostly infection in the upper lip, lower part of nose and adjoining cheek area can result in thrombosis. So these areas are called ‘dangerous area of face’.
Question 7. Describe the lymphatic drainage of the face.
Answer:
The Lymphatic Drainage Of The Face
It can be studied under three headings based on the territories of face.
- Upper territory: A greater part of the forehead, lateral halves of eyelids, conjunctiva, lateral part of cheek, and parotid area
- Middle territory: Median part of the forehead, external nose, upper lip, medial halves of the eyelid, medial part of the cheek, the greater part of jaw
- Lower territory: Central part of lower lip and chin.

Question 8. Write a note on the lacrimal apparatus.
Answer:
Lacrimal Apparatus


- It consists of structures that are involved in the secretion and drainage of lacrimal fluid
- Consist Of Mainly The Following Parts
- Lacrimal gland
- Lacrimal ducts
- Conjunctival sac
- Lacrimal puncta and lacrimal canaliculi
- Lacrimal sac
- Nasolacrimal duct.
1. Lacrimal Gland
- Serous gland situated in the lacrimal fossa on the anterolateral part of the roof of the bony orbit and upper eyelid
- Consists of an orbital part and a palpebral part
- Involved in the secretion of lacrimal fluid along with accessory lacrimal gland
- Supplied by lacrimal nerve and lacrimal branch of ophthalmic artery.
2. Secretomotor Fiers
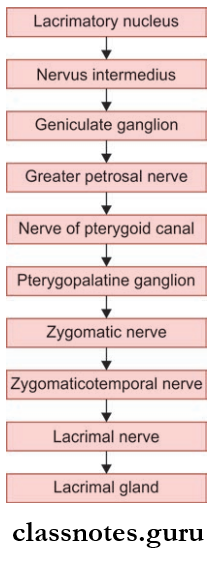
- Lacrimal Ducts: Arises from the lacrimal gland, pierce the conjunctiva of the upper lid, and opens into a conjunctival sac near the superior fornix.
- Conjunctival Sac: The space between the palpebral and bulbar conjunctiva is known as the conjunctival sac.
- Lacrimal Puncta And Canaliculi: These are small openings on the lid margin:
- Each lacrimal canaliculi begin at lacrimal punctum and is 10 mm long
- Has a vertical part 2 mm long and horizontal part 8 mm long
- Both canaliculi open into the lateral wall of sac close to each other.
- Lacrimal Sac:
- Membranous sac situated in the lacrimal groove behind medial palpebral ligament
- Upper end of the sac is blind and lower end is continuous with the nasolacrimal duct.
- Nasolacrimal Duct:
- It is an 18 mm long membranous passage
- It begin at lower end of the lacrimal sac and opens into the inferior meatus of nose
- A fold of mucous membrane forms an imperfect valve called the valve of Hasner at the lower end of duct.
Lacrimal Apparatus Applied
- For the purpose of clinical evaluation, the palpebral conjunctiva is examined for anemia and bulbar conjunctiva for jaundice.
- Excessive secretion of lacrimal fluid overflowing on the cheeks is called Epiphora and occurs as a result of an obstruction in the lacrimal fluid pathway.
- Inflammation of the conjunctiva is known as conjunctivitis and is a common disease of the eye caused due to infection or allergy.
- Inflammation of the lacrimal sac is known as dacryocystitis.
- Ducts from the orbital part traverse the palpebral part to open into the conjunctival sac. So the removal of the palpebral part is equivalent to the removal of the entire gland.
Scalp Temple And Face Multiple Choice Questions and Answers
Question 1. Which layer of scalp is regarded as the ‘dangerous layer’?
- Subcutaneous layer
- Aponeurotic layer
- Layer of loose areolar tissue
- Pericranium
Answer: 3. Layer of loose areolar tissue
Question 2. Regarding muscles of facial expression which of the following statements is incorrect:
- They are present in the superficial fascia
- They are developed from the first pharyngeal arch
- Their motor supply is derived from the facial nerve
- Morphologically they represent panniculus carnosus
Answer: 2. They are developed from first pharyngeal arch
Question 3. 26 October 2016 2:08 PMAll of the following arteries supply the anterior quadrant of the scalp except:
- Supratrochlear
- Supraorbital
- Posterior auricular
- Superficial temporal
Answer: 3. Posterior auricular
Question 4. All of the following innervate the posterior quadrant of the scalp except:
- Auriculotemporal
- Great auricular
- Greater occipital
- Lesser occipital
Answer: 1. Auriculotemporal
Question 5. Regarding the lacrimal gland which of the following statements is not correct?
- It consists of a larger orbital part and a smaller palpebral part
- It is a mucus gland
- It receives a secretomotor supply through the lacrimal nerve
- The two parts of the lacrimal glands are separated from each other by levator palpebrae superioris.
- Answer: 2. It is a mucus gland