Deep Structure Of Neck Question And Answers
Question 1. Write a note on the thyroid gland.
Answer:
Thyroid Gland
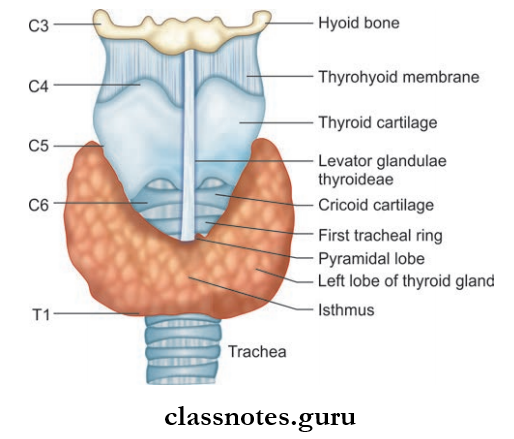


- Thyroid Gland is an endocrine gland situated in the lower part of neck
- Thyroid Gland consists of right and left lobes which are connected to each other by isthmus
- Sometimes, a third lobe may project from the isthmus upwards known as pyramidal lobe
- The Gland Secretes Hormone T3 And T4 And Calcitonin Which Are Responsible For
- Regulation of basal metabolic rate
- Stimulation of somatic and psychic growth
- Important role in calcium metabolism.
Thyroid Gland Location And Extent
- Lies in the lower part in front and sides of neck against the C5, C6, C7, and T1 vertebrae embracing the upper part of trachea.
- Each lobe extends from middle of thyroid cartilage above to the fourth or fifth tracheal ring below. The isthmus lies in front of the 2nd, 3rd, and 4th tracheal rings across the midline.
Thyroid Gland Weight And Dimensions
- The gland weighs about 25 g, which it is larger in females than males and further increases during pregnancy and menstruation.
- Each lobe measures about 5 cm × 2.5 cm × 2 cm and isthmus measures about 1.2 cm × 1.2 cm.
Thyroid Gland Capsules Of Thyroid
- Consist of an inner true capsule and outer false capsule
- True capsule is the peripheral condensation of the firous stroma of the gland
- False capsule is derived from the pretracheal fascia and is thin on the posterior surface of lobes and thick on the medial surface and forms suspensory ligament of Berry which attaches to the cricoid cartilage.
Thyroid Gland Relations
- Each lobe of thyroid gland is conical shape and has apex, base, 3 surfaces (lateral, medial, and posterolateral), and 2 borders (anterior and posterior).
- Apex is directed upwards and laterally and extends up to the oblique line of thyroid cartilage limited by attachment of sternothyroid.
- Base lies on 4th or 5th tracheal ring.
- The lateral surface is convex and is covered by strap muscle (the sternothyroid, sternohyoid, superior belly of omohyoid) and anterior border of the sternocleidomastoid.
- The medial surface is related to the trachea and esophagus, inferior constrictor and cricothyroid muscle, cricoid and thyroid cartilage, and nerves external and recurrent laryngeal nerves.
- The posterolateral surface is related to the carotid sheath and its contents.
- The anterior border is thin and related to the anterior branch of superior thyroid artery. The posterior border is thick and separates medial and posterior surfaces and is related to the inferior thyroid artery, arterial anastomoses between superior and inferior thyroid arteries, and parathyroid glands.
- The anterior surface of the isthmus is related to strap muscles (sternothyroid and sternohyoid), and anterior jugular vein.
- The posterolateral surface is related to the 2nd, 3rd, and 4th tracheal rings.
Thyroid Gland Blood Supply

- Arterial Supply: Mainly supplied by superior and inferior thyroid arteries.
- Superior Thyroid Artery:
- A branch of external carotid artery
- It runs downwards and forwards along with external laryngeal nerve and pierces pre tracheal fascia to reach upper pole of the lobes and divides to anterior and posterior branches.
- Anterior branch descends along anterior border and continues along upper border of isthmus to anastomose with its fellow of opposite side.
- Posterior branch descends along posterior border and anastomose with the ascending branch of inferior thyroid artery.
- Inferior Thyroid Artery:
- A branch of thyrocervical trunk which runs along the medial border of the scalenus anterior and passes medially behind the carotid sheath to reach back of the gland.
- It divides into 4–5 glandular branches which pierce fascia and reach the lower part of the gland.
- One ascending branch anastomoses with the posterior branch of the superior thyroid artery and supplies the parathyroid gland.
- In 3% of individuals, an artery arises from the brachiocephalic trunk/directly from arch of aorta called thyroid ima artery which enters into the lower part of isthmus.
- Accessory thyroid arteries arising from esophageal and tracheal arteries also supply the gland.
- Superior Thyroid Artery:
Thyroid Gland Venous Drainage: Drained by superior, middle, and inferior thyroid veins.
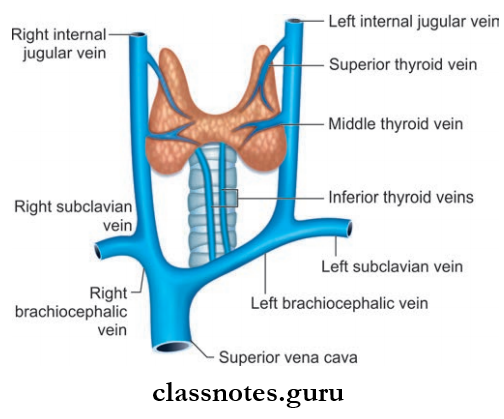
- Superior Thyroid Vein: Usually emerges at the upper pole and passes along with superior thyroid artery and drains into the internal jugular vein.
- Middle Thyroid Vein: Emerges at middle of the lobe and drains to internal jugular vein.
- Inferior Thyroid Vein: Emerge at the lower border of isthmus and in front of the trachea they form a plexus and drain to left brachiocephalic vein.
- Throid veins of Kocher emerge between middle and inferior thyroid veins drain to internal jugular vein.
Thyroid Gland Lymphatic Drainage
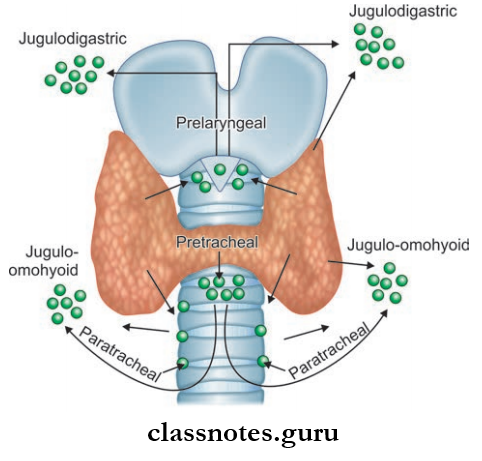
Lymphatic Drainage Of Thyroid Gland

Thyroid Gland Nerve Supply
- Nerves are derived from middle cervical ganglia mainly.
- The gland also receives supply from superior and inferior cervical ganglia.
Thyroid Gland Microscopy: Presence of two types of secretory cells:
- Follicular Cells: Responsible for secretion of T3, T4.
- Parafollicular Cells: Responsible for secretion of calcitonin.
Thyroid Gland Development
- After the formation of pharyngeal arches, the medial ends of mandibular arches are separated by a midline swelling called tuberculum impar.
- Just behind the tuberculum, the flor of the pharynx shows a thickening in the middle line which soon gets depressed to form a diverticulum called the thyroglossal duct.
- The site of origin of the thyroglossal duct is seen as a depression called foramen cecum.
- The thyroglossal duct growns down in midline into the neck and its tip bifurcates.
- The cells of the bifid end proliferate to form the two lobes of thyroid gland.
- The parafollicular cells develop from the caudal pharyngeal complex which is derived from fourth and fifth pharyngeal pouches.
Thyroid Gland Applied
- The ligament of Berry holds the thyroid gland firmly in contact with larynx and prevents the sliding even when it is enlarged.
- The thyroid gland moves up and down during swallowing because of its fascial capsule attached to the thyroid cartilage.
- The venous plexus lies deep to the true capsule. So, in surgeries thyroid gland is removed along with true capsule to avoid injuries to the venous plexus.
- Thyroid gland can be found at an abnormal position along the course of the thyroglossal duct. This can be under the mucosa of the dorsum of tongue (lingual thyroid), within substance of the tongue, above the hyoid bone, or may even be intrathoracic.
- In case of hyperthyroidism, the thyroid gland is removed with true capsule, and the procedure is known as a thyroidectomy. The thyroidectomy can be total, subtotal, or near-total thyroidectomy.
- Dense venous plexus are present deep to the true capsule, so in thyroidectomy gland is removed along with the true capsule to avoid hemorrhage.
- During thyroidectomy, superior thyroid artery is ligated near the gland to save the external laryngeal nerve and the inferior thyroid artery is ligated away from the gland to save the recurrent laryngeal nerve.
- Simple goiter is the enlargement of the gland without any signs of hyperthyroidism and occurs due to defiiency of iodine in diet.
- Tumors of the gland can spread to neighboring structures and may cause compression of structures like trachea and nerves.
Question 2. Write a short note on parathyroid glands.
Answer:
Parathyroid Glands

- Two pairs of small endocrine glands present on the posterior border of thyroid gland
- Responsible for secretion of hormone parathormone which controls the metabolism of calcium and phosphorous along with calcitonin.

Parathyroid Glands Location
- Superior parathyroid usually lies on the middle of posterior border of thyroid gland dorsal to the recurrent laryngeal nerve.
- Position of the inferior parathyroid is variable as they can be present:
- Within the false capsule below the inferior thyroid artery
- Behind and outside false capsule just above the inferior thyroid artery
- Within substance of thyroid gland.
Parathyroid Glands Weight And Dimension
- Each gland weighs about 50 mg
- It is oval in shape and measures 6 mm × 4 mm × 2 mm.
Parathyroid Glands Blood Supply
- Arterial Supply
- Mainly by inferior thyroid artery
- Also from anastomosis between superior and inferior thyroid artery.
- Venous Drainage: By veins associated with the thyroid gland, i.e. superior, middle, and inferior thyroid vein.
Parathyroid Glands Lymphatics: Lymph nodes associated with the thyroid gland drains the parathyroid.
Parathyroid Glands Nerve Supply: Vasomotor nerves derived from middle and superior cervical ganglia.
Parathyroid Glands Development
- Superior Parathyroid: Endoderm of the fourth pharyngeal pouch.
- Inferior Parathyroid: Endoderm of third pharyngeal pouch.
- During development, the thymus gland (which develops from third pouch) descends downwards to thorax.
- Since the parathyroid glands derived from third pouch are in close relation with thymus, it is carried with the thymus for some distance. On the other hand, the parathyroid glands derived from the fourth pouch are prevented from descending caudally.
- As a result, the parathyroids derived from the fourth pouch become the superior parathyroid and those derived from third pouch become inferior parathyroid glands.
Parathyroid Glands Applied
- Hypoparathyroidism occurs as a result of the inadvertent removal of parathyroid glands during thyroidectomy.
- Parathyroid insufficiency results in tetany which is characterized by carpopedal spasms, convulsions, and low serum calcium.
- Hyperparathyroidism occurs as a result of tumors of parathyroid glands.
- Excess of parathormone causes rise in blood calcium leading to the fragility of bones and proneness to fractures.
Question 3. Write A Short Note On The Thymus.
Answer:
Thymus
- Thymus is a lymphoid organ situated in the anterior and superior mediastinum of thorax extending to the lower part of neck.
- Thymus is welldeveloped at birth and grows up to puberty and undergoes gradual atrophy thereafter and is later replaced by fat.
Thymus Weight And Dimension
- Thymus Weight And Dimension is a bilobed structure, made of two pyramidal lobe of unequal size connected by areolar tissue.
- Thymus Weight And Dimension weighs about 10–15 g at birth, 30–40 g at puberty, and 10 g after midadult life.
Thymus Blood Supply
- Supplied by internal thoracic and inferior thyroid artery.
- Drained by left brachiocephalic, internal thoracic, and inferior thyroid vein.
Thymus Nerve Supply: Vasomotor nerves are derived from stellate ganglion.
Thymus Function
- Involved in lymphopoiesis, as this is a primary lymphoid organ.
- Site of maturation of T lymphocytes.
Thymus Development: Develops from the third pharyngeal pouch.
Thymus Applied
- In patients with thymic aplasia, agenesis or hypoplasia lymphopenia occurs and leads to decreased immunity and death early due to infections.
- One of the severe forms of T cell immunodeficiency is DiGeorge syndrome.
- The epithelial cell tumor of the thymus is known as thymoma and when large in size, can compress structures like the trachea, esophagus, and large veins in the superior mediastinum.
Question 4. Write a short note on the lymph nodes of head and neck.
Answer:
The lymph Nodes Of Head And Neck


- The lymph nodes of head and neck can be studied under two headings:
- Peripheral nodes or superficial nodes
- Deep cervical nodes
- The entire lymph from head and neck region ultimately drain into deep cervical nodes either directly or through peripheral nodes.
Peripheral Or Superficial Nodes: The peripheral nodes can be arranged as superficial circles or deep circle.
The superficial Circle Consists Of:
- Submental Nodes
- Lie deep to chin
- Drain from tip of the tongue and the anterior part of the floor of mouth
- Submandibular Nodes: Drain lateral surface of the tongue, lower gum, teeth, and central area of the forehead
- Buccal And Mandibular Nodes
- Buccal nodes lie on the buccinator and mandibular node at the lower border of mandible near the anteroinferior angle of the masseter
- They drain part of the cheek and lower eyelids
- Efferent pass to the superior group of deep cervical nodes.
- Preauricular Nodes: Drain parotid gland, temporal region, and middle ear.
- Postauricular Nodes
- Lie on mastoid process
- Drain a part of the scalp above, behind the auricle, posterior wall of the external acoustic meatus.
- Occipital Nodes
- Lie at the apex of the posterior triangle
- Drain occipital region of the scalp.
- Anterior Cervical Nodes
- Lie along anterior jugular vein
- Drain skin of anterior part of neck.
- Superficial Cervical Nodes
- Lie along external jugular vein
- Drain lobule of the auricle, flor of external acoustic meatus and skin over parotid, and angle of jaw.
The Deep Circle Consists Of:
- Prelaryngeal And Paratracheal Nodes:
- Lie deep to investing layer of deep fascia on the cricothyroid membrane and in front of trachea respectively
- Drain the larynx, trachea, and isthmus of thyroid
- Paratracheal Nodes
- Lie on the sides of the trachea and esophagus
- Drain esophagus, trachea, and larynx
- Retropharyngeal Nodes
- Lie in between the prevertebral and buccopharyngeal fascia covering the posterior wall of the pharynx
- Drain pharynx, soft palate, part of the hard palate, and auditory tube.
Deep Nodes
For convenience, deep cervical lymph nodes can be grouped as superior and inferior group, even though there is no sharp/clear demarcation between them.
- Superior Group
- Lie above omohyoid
- Main lymph node of the group is the jugulodigastric node present below the posterior belly of digastric and between the angle of the mandible and the anterior border of the sternocleidomastoid
- It drains from the palatine tonsil.
- Inferior Group
- Present below omohyoid muscle
- The main lymph node of the group is the jugulo-omohyoid lymph node which is present just above the intermediate tendon of the omohyoid deep to the sternocleidomastoid
- It mainly receives lymph from the tongue.
- The supraclavicular nodes are present in the lower part of the posterior triangle and are related to subclavian vessels.
- The left supraclavicular lymph nodes are known as Virchow’s nodes.
- The deep cervical lymph nodes receive lymph from the entire head and neck.
- The efferents from the deep group form the jugular lymph trunk on each side and terminate into the right lymphatic duct on the right side and thoracic duct on the left side.
Lymph Nodes Of Head And Neck Applied
- Cervical lymph nodes are enlarged in diseases of the lymphatic system, like Hodgkin’s disease, inflmmatory conditions like tuberculosis, and other malignancies.
- In carcinomas of the stomach, colon, testis, etc. causes enlargement of Virchow’s node due to retrograde spread through thoracic duct.
- Confirmation of clinical diagnosis is made by doing a cervical node biopsy.
Question 5. Write a short note on scalene muscles.
Answer:
Scalene Muscles


- These are the paravertebral muscles of neck
- These muscles extend from the transverse process of cervical vertebrae to the first two ribs
- They elevate ribs or bend the cervical part of the vertebral column laterally.
Scalenus Anterior
- Key Muscle Of Neck
- Origin: Anterior tubercles of transverse processes of 3rd to 6th cervical vertebrae.
- Insertion
- Scalene tubercles on the inner margin of 1st rib
- Adjoining ridge on the superior surface of 1st rib.
- Nerve Supply: Ventral rami of C4–C6 nerves.
- Action
- When both act together—the muscles fi the first rib during quiet and forced inspiration
- When acting singly—it bends neck forwards or laterally turning face to the opposite side.
Scalene Muscles Relations
- Anterior
- Phrenic nerve covered by prevertebral fascia
- Lateral part of carotid sheath
- Sternocleidomastoid
- Clavicle.
- Posterior
- Brachial plexus
- Subclavian artery
- Scalenus medius
- Cervical pleura.
- Medial Border: Forms the lateral margin of scalenovertebral triangle which contains vertebral artery thyrocervical trunk, sympathetic chain, brachiocephalic vein, and thoracic duct on left side.
- Lateral Border: Related to trunks of brachial plexus and subclavian artery.
Scalene Muscles Scalenus Medius
- Origin
- Posterior tubercles of 2nd–7th cervical vertebrae
- Transverse process of the axis.
- Insertion: Superior surface of the first rib posterior to groove for subclavian artery.
- Nerve Supply: Ventral rami of C3–C8 nerves.
- Action
- Lateral flexion of the cervical spine
- Elevates first rib during forceful inspiration.
Scalene Muscles Scalenus Posterior
- Origin: Posterior tubercles of transverse process of C4– C6 vertebrae
- Insertion: Outer surface of 2nd rib behind tubercle for serratus anterior
- Nerve Supply: Ventral rami of C6–C8 nerves
- Action
- Lateral flexion of cervical spine
- Elevation of 2nd rib during forceful inspiration.
Scalene Muscles Scalenus Minimus: Also known as Scalenus pleural
- Origin: Transverse process of 7th cervical vertebra
- Insertion: Inner border of fist rib few fibers of the muscle are continuous with the subpleural membrane (Sibson’s fascia) and cervical pleura. The subpleural membrane is regarded as the flattened tendon of this muscle.
- Action: Pulls the dome of the cervical pleura.
Scalene Muscles Applied
- Scalenius Anterior Syndrome: Hypertrophy or spasm of scalenus anterior muscle may compress the contents of scalene triangle.
- Division of the muscle is done to relieve the symptoms.
Question 6. Write A Short Note On Cervical Pleura.
Answer:
Cervical Pleura: Covers the apex of lung.
Cervical Pleura Extent
- Rises into the root of the neck 5 cm above the 1st costal cartilage and 2.5 cm above the medial onethird of clavicle.
- Cervical Pleura Extent is strengthened by a subpleural membrane so that the root of neck is not puffed up and down during respiration.
Cervical Pleura Relations: Relations of cervical pleura
- Anterior
- Subclavian artery and branches
- Scalenus anterior
- Posterior
- Sympathetic trunk
- 1st posterior intercostal vein
- Superior intercostal artery
- First thoracic nerve
- Lateral
- Scalenus medius
- Lower trunk of brachial plexus
- Medial
- Vertebral bodies
- Esophagus
- Trachea
- Left recurrent laryngeal nerve
- The thoracic duct is on the left side.
Question 7. Write a short note on the styloid apparatus.
Answer:
Styloid Apparatus

- The stylohyoid ligament is attached to the tip, the styloglossus muscle to the anterior aspect (lower part), the stylohyoid muscle to the posterior aspect (upper part), and the stylopharyngeus to the medial aspect
- The styloid process with its attached structures is called the styloid apparatus.
The Attached Structures Include:
- 3 muscles: Stylohyoid, styloglossus, stylopharyngeus
- 2 ligaments: Stylohyoid, stylomandibular.
Styloid Apparatus Origin
- Syloid process, stylohyoid ligament, and muscle from 2nd branchial arch.
- Stylopharyngeus: 3rd arch
- Styloglossus: Occipital myotomes
- Stylomandibular ligament from deep fascia of neck.
Styloid Apparatus Features
- Styloid Process
- Long slender bony process projecting downwards, forwards, and medially from the temporal bone
- Descends between external and internal carotid arteries to reach side of pharynx
- Interposed between the parotid gland and internal jugular vein
- The attachments resemble the reins of the chariot of which ligaments are nonadjustable and muscles are adjustable.
- Styloglossus Muscle: Arises from the anterior surface of the styloid process and is inserted to side of the tongue.
- Stylopharyngeus Muscle: Arises from the medial surface of base of the styloid process and is inserted to the posterior border of the lamina of thyroid cartilage.
- Stylohyoid Muscle: Extends between the posterior surface of the styloid process and muscles to the hyoid bone.
- Stylohyoid Ligament: Extended from the tip of the styloid process to lesser cornu of the hyoid bone.
- The stylomandibular ligament attaches laterally to the styloid process above and angle of mandible below.
Styloid Apparatus Applied
- In case of some individuals elongation of the styloid process and stylohyoid ligament, calcification occurs and this condition is known as Eagle syndrome.
- The tissues in the throat rub on the styloid process during the act of swallowing with resulting in pain along the glossopharyngeal nerve. There is also pain upon turning the head or extending the tongue.
Deep Structure Of Neck Multiple Questions And Answers
Question 1. Select the incorrect statements regarding internal jugular vein.
- It begins as the direct continuation of the sigmoid sinus
- It presents 2 dilatations
- It is crossed by 2 muscles on its superficial aspect
- Its lower part lies in the greater supraclavicular fossa
Answer: 4. Its lower part lies in the greater supraclavicular fossa
Question 2. The inferior thyroid artery is a branch of:
- External carotid artery
- Internal carotid artery
- Throcervical trunk
- Brachiocephalic trunk
Answer: 3. Throcervical trunk
Question 3. The thyroid venous plexus lies:
- Between true and false capsules of the thyroid gland
- Deep to true capsule
- Outside false capsule
- Within the substance of the gland
Answer: 2. Deep to true capsule
Question 4. Select the true statement about the inferior parathyroid gland:
- It develops from the third pharyngeal pouch
- It develops from the fourth pharyngeal pouch
- It is more constant in position compared to the superior parathyroid gland
- It is closely related to the external laryngeal nerve
Answer: 1. It develops from the third pharyngeal pouch
Question 5. Select the incorrect statement about the cervical plexus:
- It is formed of the ventral rami of C1 to C4 cervical spinal nerves
- It is called the plexus of loops
- It is superfiial to prevertebral fascia
- Its superficial branches are cutaneous in nature.
Answer: 3. It is superficial to the prevertebral fascia
