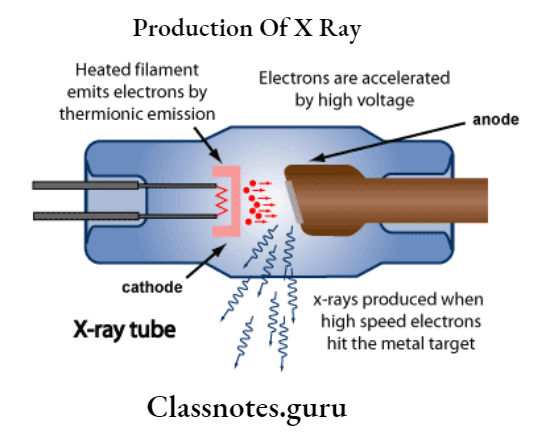
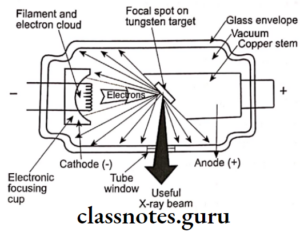
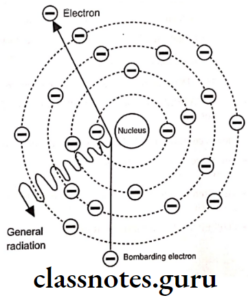
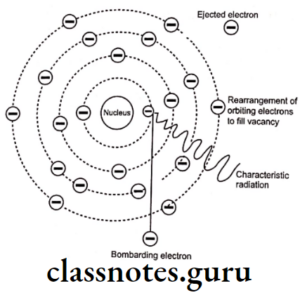
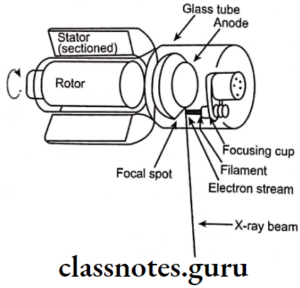
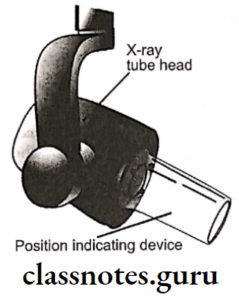
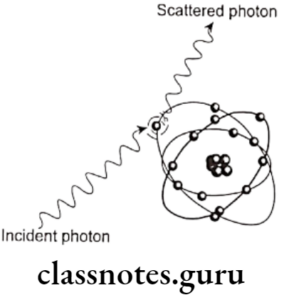
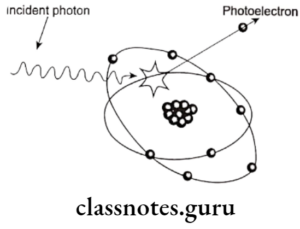
X-Ray Film And Accessories Important Notes
- Half value layer {HVL} characterizes the penetrating quality of x-ray beam.
- HLV is the thickness of aluminium required to reduce half the number of X-ray photons passing through it.
- Aluminium filter selectively removes the less penetrating photons, which only contributes to patient exposure and doesn’t have enough energy to reach the film.
- Its thickness is 1.5 mm for 70 kVp.
- Collimator is a radiopaque material (usually lead), which reduces the size of X-ray beam.
- Thus it reduces patient exposure and increase quality of X-ray film by reducing the formation of scattered radiation and penumbra.
- X-ray beam is collimated to a circle of 2.75 inches or 7cm.
- IOPA film
- Size – 0 – 22 x 35 mm – For small children
- Size – 1 – 24 x 40 mm – For anterior projection
- Size – 2 – 32 x 41 mm – For adults
- Bitewing film
- Size – 0 – For very small children
- Size – 1 – Children
- Size – 2 – For adults
- Occlusal film
- 3 times larger than a size 2 film – 57 x 76 mm
- Screen film
- 8 x 10 inches – for extra oral projection along with the intensifying screen
- Composition of film
- Emulsion:
- It is sensitive to X-rays and visible light
- It records the image
- It consists of:
- Silver halide crystals
- Gelatin matrix
- Base:
- It is made up of polyethylene terephthelate (polyester)
- Adhesive layer:
- It is applied to base before emulsion is applied for proper adaptation
- Emulsion:
X-ray film and accessories notes
- Film packet
- It consists of:
- An outer plastic wrapping
- It is made of white paper or soft vinyl
- It has two sides: label side and tube side
- The label side has a flap to open the film packet
- A thin sheet of lead foil
- It is placed in the plastic wrapper
- It absorbs most of the X-rays which pass through the film
- A sheet of black paper
- It protects the film from any light leak
- X-ray film
- It has rounded corners and an embossed raised dot for orientation
- It consists of:
- Types of collimator
- Diaphragm
- Tubular
- Rectangular
- Diaphragm
- Types of filtration
- Inherent filtration
- External filtration
- Types of intensifying screens
- Blue emitting visible light
- Green emitting visible light
- Composition of intensifying screen
- Base
- It is made of polyester plastic with 0.25 mm thickness
- Reflecting layer
- It is made up of titanium dioxide coated on the base material and lies below the phosphor layer
- Protective coat
- It is made of plastic about 8 mm thickness placed over the phosphor layer to provide protection for the phosphor layer
- Base
- Types of grid
- Stationary grids
- Parallel grids
- Focused grids
- Moving grids
- Potter bucky grids
- Stationary grids
Read And Learn More: Oral Radiology Question and Answers
X-Ray Film And Accessories Short Essays
Question 1. Collimation and filtration. Or Collimator
Answer:
Collimation:
- When an X-ray beam is directed at the patient, 90 percent of the X-ray photons are absorbed by the tissues and remaining 10 percent pass through as the information carrying beam results in the formation of image on a film
- Many of the absorbed photons generate scattered radiation that travels in all directions results in film fog which degrades the image contrast
- To reduce a lead collimator in the path of the X-ray beam can be placed
- Collimation means reducing the size of the X-ray beam by placing a radiopaque barrier containing aperture in the path of beam and thus reduces the volume of irradiated tissue by absorbing scattered radiation
- Thus it reduces patient exposure and increases the film quality
- Collimator is the device which collimates the X-ray beam thus reduces the formation of scattered radiation
Collimation Types:
- Diaphragm
- Tubular
- Rectangular
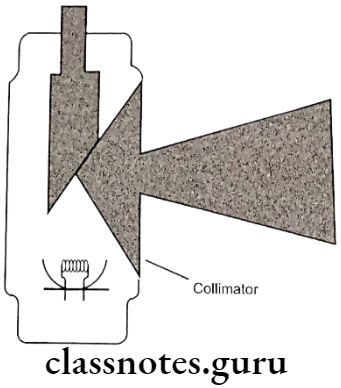
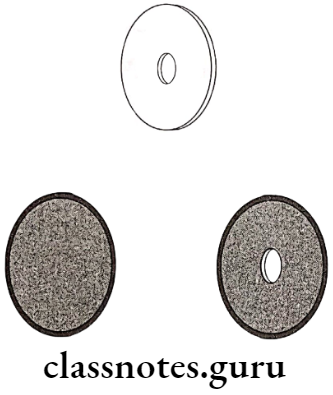
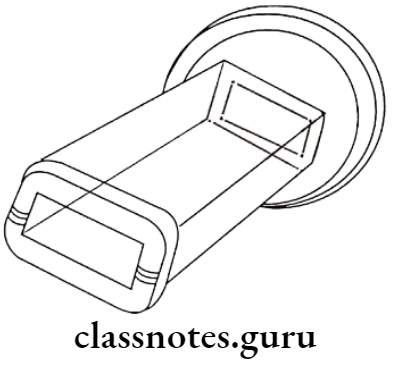
Filtration:
- X-ray beam emitted from the X-ray tube consists of not only high energy but also of low energy photons
- Low-energy photons have little penetrating power
- They are absorbed within the tissues causing hazards to the patient and give no contribution to image formation
- The purpose of adopting filtration is to selectively remove these low-energy photons from the X-ray beam by placing an aluminum filter in the path of the beam
- It also allows high-energy photons to pass through which results in reduced patient exposure
Filtration Types:
- Inherent filtration:
- This filters the X-ray beam within X-ray machine by glass wall of the X-ray tube, insulating oil that surrounds the X-ray tube and barrier material that prevents the oil escaping out
- External filtration:
- External filtration is applied in the form of aluminum discs placed in the path of the beam
Radiographic film and accessories short notes
Question 2. X-Ray Film.
Answer:
X-Ray Film
It is a type of photographic film.
X-Ray Film Types:
- Intraoral films
- Extraoral films
X-Ray Film Composition:
- Emulsion:
- It is sensitive to X-rays and visible light
- It records the image
- It consists of:
- Silver halide crystals
- They are composed of mainly silver bromide and lesser content of silver iodide which are photosensitive
- Each silver grain diameter is 1.8 μm
- Gold may be added to improve its sensitivity
- Gelatin matrix
- It suspends silver halide crystals evenly in the gel made from cattle bone
- It absorbs the processing solution
- Thus allows the chemicals to react with silver halide crystals
- Silver halide crystals
X-Ray Film Base:
- It is made up of polyethylene terephtlelate (polyester)
- Its diameter is 0.18 mm
- The function of the base is to support the light sensitive silver halide crystals
- Base is slightly blue tint to enhance the image quality
- Its translucency cast no pattern on the resultant radiograph
- It with stands exposure during processing without distortion
- It is flexible for proper handling
X-Ray Film Adhesive layer:
- It is applied to base before emulsion is applied for proper adaptation
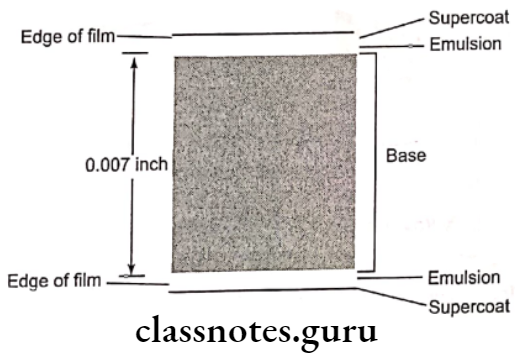
X-Ray Film Sizes:
- Periapical radiograhic films:
- Size 0: small children, 22 x 35 mm
- Size 1: children, 24 x 40 mm
- Size 2: adult, 31 x 41 mm
- Occlusal films:
- Size: 57 x 76 mm
X-ray film types and components
Question 3. Film Packet.
Answer:
Film Packet
- It consists of:
- An outer plastic wrapping
- It is made of white paper or soft vinyl
- It is sealed, semistiff, moisture proof, light proof and clear
- It should be directed towards the tube
- It protects the film from exposure to light and saliva
- It has two sides: label side and tube side
- The label side has a flap to open the film packet
- An embossed dot is present for positioning the film
- The dot must be placed occlusally
- An outer plastic wrapping

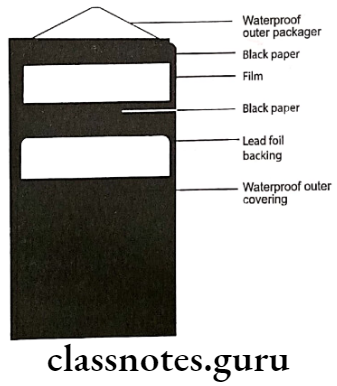
- A thin sheet of lead foil
- It is placed in the plastic wrapper
- It absorbs most of the X-rays which pass through the film
- Thus prevents the soft tissues from it
- It absorbs the back scattered radiation
- It prevents fogging
- A sheet of black paper
- It protects the film from any light leak
- X-ray film
- It has rounded corners and an embossed raised dot for orientation
- A thin sheet of lead foil
Question 4. Intensifying Screens.
Answer:
Intensifying Screens
These are image receptors used in combination with the X-ray film for all extraoral radiographic procedures such as panoramic, cephalometric and skull radiography
Intensifying Screens Types:
- Blue emitting visible light
- Green emitting visible light
Intensifying Screens Mechanism:
- Intensifying screens contain various inorganic salts or phosphors would fluoresce when exposed to a X-ray beam
- The intensity of it is directly proportional to intensity of the X-ray beam, which strikes the phosphors crystals
- Each X-ray photon convert into multiple visible light which strikes the X-ray film thus reducing amount of radiation required to expose film
- But it results in loss of fine detail on image because of dispersion of visible lights from phosphor crystals
Intensifying Screens Composition:
- Base:
- It is made of polyester plastic with 0.25 mm thickness
- It provides mechanical support for the intensifying screen
- Reflecting layer:
- It is made up of titanium dioxide coated on the base material and lies below the phosphor layer
- The main function is to reflect any visible light emitted from the phosphor layer back to the film
- Devoid of this layer is to get sharpness of the image because this layer produce divergence of the visible light reflected back to the film causing unsharpened image
- Phosphor layer:
- It is composed of light sensitive phosphor crystals suspended in a plastic material
- When the phosphors are struck by X-ray photons they emit visible light that exposes the X-ray film
- Protective coat:
- It is made of plastic about 8 mm thickness placed over the phosphor layer to provide protection for the phosphor layer
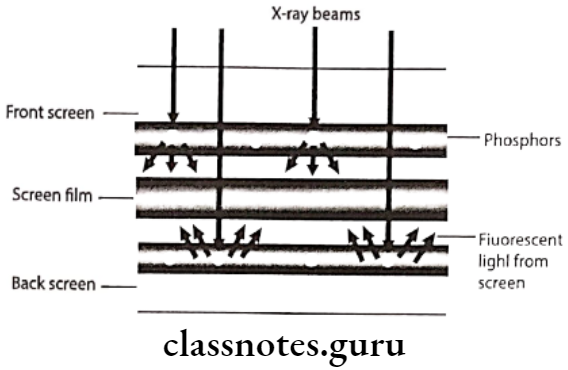
X-ray film and accessories in radiology
Question 5. Grids.
Answer:
Grids
It is a device which consists of an alternative strip of radiopaque and radiolucent material which is placed between the object and the film to improve the quality of the image by removal of scattered radiation that causes fog and reduces film contrast
Composition:
- It is composed of alternate strips of radiopaque that are lead and radiolucent often plastic
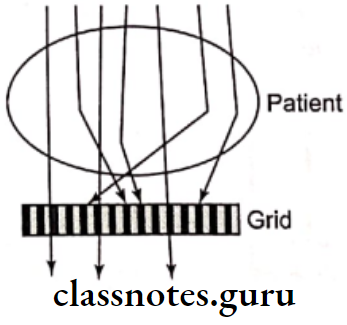
Grids Functions:
- When the X-ray photons hit the object secondary photons are generated and they are scattered towards the film
- These scattered photons are deviated in their direction of travel from that of primary beam would cause film fog and reducing the film contrast
- Grids are placed between the object and the film absorbs all scattered radiation that are deviated from the primary beam by radiopaque material and allow only the primary beam through the radiolucent material of plastic into the films
Grids Types:
- Stationary grids:
- Parallel grids
- Focused grids
- Moving grids:
- Potter bucky grids
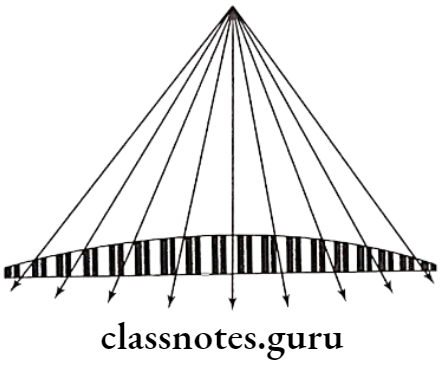
Question 6. Potter Bucky Grid.
Or
Potter bucky diaphragm.
Answer.
Potter Bucky Grid
- In this the grid is moved sideways across the film during exposure
- This leads to the blurring out of the shadows of grid strips
- Thus they are not visible on the film
- The image of the radiopaque grid lines on the film can be deleted by mechanically moving the grid in the direction of 90 degree to the grid lines during exposure
- This results in blurring out of radiolucent lines
- Results in uniform exposure
- It does not interfere with the absorption of scattered radiation
Question 7. Filtration.
Answer.
Filtration
- X-ray beam emitted from the X-ray tube consists of not only high energy but also of low energy photons
- Low energy photons have little penetrating power
- They are absorbed within the tissues causing hazards to the patient and gives no contribution to image formation
- The purpose of adopting filtration is to selectively remove these low energy photons from the X-ray beam by placing an aluminium filter in the path of the beam
- It also allows high energy photons to pass through which results in reduced patient exposure
Filtration Types:
- Inherent filtration:
- This filters the X-ray beam within X-ray machine by glass wall of the X-ray tube, insultating oil that surrounds the X-ray tube and barrier material that prevents the oil escaping out
- External filtration:
- External filtration is applied in the form of aluminium discs placed in the path of the beam.
Dental X-ray film and accessories notes
X-Ray Film And Accessories Short Answers
Question 1. Composition of X-Ray Film.
Answer:
Composition of X-Ray Film
It is a type of photographic film.
X-Ray Film Types:
- Intraoral films
- Extraoral films
X-Ray Film Composition:
Emulsion:
- It is sensitive to X-rays and visible light
- It records the image
- It consists of:
- Silver halide crystals
- They are composed of mainly silver bromide and lesser content of silver iodide which are photosensitive
- Each silver grain diameter is 1.8 μm
- Gold may be added to improve its sensitivity
- Gelatin matrix
- It suspends silver halide crystals evenly in the gel made from cattle bone
- It absorbs the processing solution
- Thus allows the chemicals to react with silver halide crystals
- Silver halide crystals
X-Ray Film Base:
- It is made up of polyethylene terephtlelate (polyester)
- Its diameter is 0.18 mm
- The function of the base is to support the light sensitive silver halide crystals
- Base is slightly blue tint to enhance the image quality
- Its translucency cast no pattern on the resultant radiograph
- It with stands exposure during processing without distortion
- It is flexible for proper handling
X-Ray Film Adhesive layer:
- It is applied to base before emulsion is applied for proper adaptation

Film Sizes:
- Periapical radiographic films:
- Size 0: small children, 22 x 35 mm
- Size 1: children, 24 x 40 mm
- Size 2: adult, 31 x 41 mm
- Occlusal films:
- Size: 57 x 76 mm
X-ray cassettes and screens short essay
Question 2. Composition of Intensifying Screens.
Answer:
Composition:
Base:
- It is made of polyester plastic with 0.25 mm thickness
- It provides mechanical support for the intensifying screen
Reflecting layer:
- It is made up of titanium dioxide coated on the base material and lies below the phosphor layer
- The main function is to reflect any visible light emitted from the phosphor layer back to the film
- Devoid of this layer is to get sharpness of the image because this layer produce divergence of the visible light reflected back to the film causing unsharpened image
Phosphor layer:
- It is composed of light sensitive phosphor crystals suspended in a plastic material
- When the phosphors are struck by X-ray photons they emit visible light that exposes the X-ray film
Protective coat:
- It is made of plastic about 8 mm thickness placed over the phosphor layer to provide protection for the phosphor layer

Radiographic film and intensifying screen essay
Question 3. Collimation
Answer:
Collimation
- When an X-ray beam is directed at the patient, 90 percent of the X-ray photons are absorbed by the tissues and remaining 10 percent pass through as the information carrying beam results in the formation of image on a film
- Many of the absorbed photons generate scattered radiation that travels in all directions results in film fog which degrades the image contrast
- To reduce a lead collimator in the path of the X-ray beam can be placed
- Collimation means reducing the size of the X-ray beam by placing a radiopaque barrier containing aperture in the path of beam and thus reduces the volume of irradiated tissue by absorbing scattered radiation
- Thus it reduces patient exposure and increases the film quality
- Collimator is the device which collimates the X-ray beam thus reduces the formation of scattered radiation
Types:
- Diaphragm
- Tubular
- Rectangular



X-ray film construction and types
Viva Voce
- For a given beam the intensity is inversely proportional to the square of the distance from the source
- Base of x-ray film is composed of polyester polyethylene teraphalate
- Emulsion of x-ray film consists of gelatin and silver halide
- Intensifying screen is composed of base, titanium oxide, phosphor and protective coat
- Potty Bucky diaphragm absorbs scattered radiation