Asepsis In Endodontics Definitions
- Sterilization
- It is the complete destruction of agents that are capable of causing infections, including spores.
Asepsis In Endodontics Important Notes
- Methods of sterilization
- Physical agents
- Sunlight
- Drying
- Dry heat
- Moist heat
- Filtration
- Radiation
- Chemical agents
- Alcohol
- Aldehyde
- Chlorines
- quaternary ammonium compound
- Phenolic compounds
- Antiseptics
- Physical agents
Asepsis In Endodontics
Asepsis In Endodontics Long Essays
Question 1. Discuss sterilization of endodontic instruments.
Answer.
Sterilization: It is the complete destruction of agents that are capable of causing infections, including spores.
Read And Learn More: Endodontics Question and Answers
Sterilization Of Endodontic Instruments Methods:
Physical Agents:
- Sunlight:
- Natural means
- Has bactericidal activity
- Drying:
- Unreliable
- Spores are unaffected
- Dry Heat:
- Consists of
- Flaming – for culture tubes, glass
- Red heat – needles
- Incineration – Dressings
- Hot air oven – At 160°C for 2 hours
- Metallic, glass particles, powder
- Consists of
- Moist Heat:
- Causes denaturation of proteins
- Filtration:
- Radiation:
- Causes:
- Inhibition of DNA replication
- Damaging structure of DNA
- Denaturation of protein
- Causes:
- Ultrasonic Vibration:
Sterilization Of Endodontic Instruments Chemical agents:
- Alcohol Ex. Ethyl alcohol
- Bactericidal
- Corrosive
- Fast acting
- Aldehyde – Ex.Glutaraldehyde
- High-level disinfectant
- Non-corrosive
- Long activated life
- Chlorines
- Quaternary Ammonium Compound
Ex:- Benzalkonium chloride
- Low-level disinfectant
- Phenolic compounds:
- Low-level disinfectant
- Used for floors, walls, and furniture
- Antiseptics
- Iodophor Ex. Povidoneiodone
- Broad spectrum
- Formulated as 1% I2 solution
- Chlorhexidine
- Iodophor Ex. Povidoneiodone
Sterilization Of Endodontic Instruments:
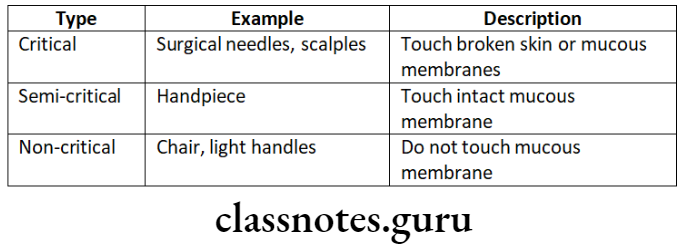
Sterilization In Endodontics
Sterilization Of Endodontic Instruments Steps:
- Pre-soaking in water to soften organic debris
- Cleaning – Hand washing or ultrasonic cleaning is done
- Drying – To prevent corrosion
- Packaging – Wrapping of instruments in clothes
- Sterilization
- Drying/cooling
- Storage
- Distribution
- Sharpening of instruments
Asepsis In Operative Dentistry
Asepsis In Endodontics Short Questions And Answers
Question 1. Disinfection.
Answer.
Disinfection
- It is the destruction of pathogenic micro-organisms
- It permits adequate removal of pulp tissue and debris
- This leads to the enlarging of the canal by biomechanical means and the clearing of its contents by irrigation
Question 2. Glass Bead Sterilizer/Salt Bead Stabilizer.
Answer.
Glass Bead Sterilizer
Rapid method of sterilization
Glass Bead Sterilizer Materials Used:
- Usually salt
- Salt is replaced by glass beads smaller than 1 mm in diameter
Glass Bead Sterilizer Reason For Smaller Beads:
- Efficient in transferring heat to instruments
- Time required – 5-15 seconds
- Temperature – 437 – 465°F
Glass Bead Sterilizer Advantages:
- Easily available
- Salt is replaced by glass beads smaller than 1 mm in diameter
Glass Bead Sterilizer Disadvantage:
- Handle portion is not sterilized
Endodontic Disinfection Methods
Question 3. Autoclave.
Answer.
Autoclave
Moist heat sterilization method
Autoclave Principle:
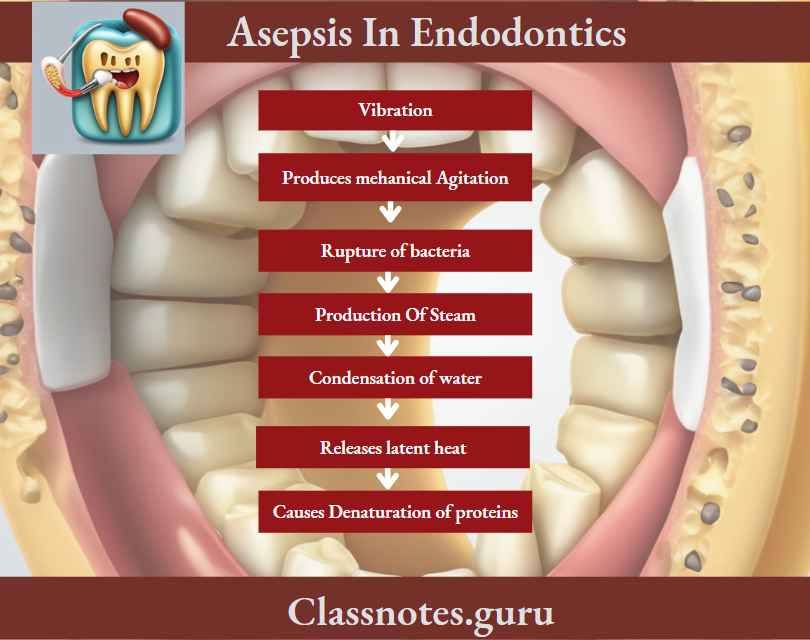
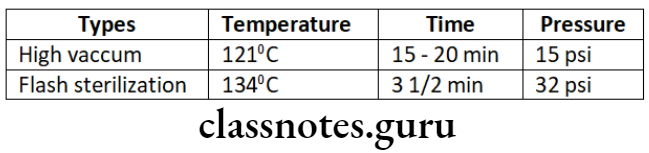
Autoclave Advantages:
- Effective
- Accurate
- Rapid
Autoclave Disadvantages:
- Causes corrosion
- Melts rubber
- Unsuitable for oils
Autoclave Factors Effecting It:
- Cleaning of instruments
- Direct flow of steam
- Periodic monitoring of sterilizer
Asepsis In Operative Dentistry
Asepsis In Endodontics Viva Voce
- The hottest part of the glass bead sterilizer is along its outer rim and the temperature is lowest in the center of the surface layer of salt
