Oral Medicine Periodontal Disease Important Notes
1. Widening Of PDL Space Is Seen In
- Osteosarcoma
- Chondrosarcoma
- Scleroderma
- Trauma from occlusion
2. Obliteration Of PDL Space Is Seen In
- Hypercementosis
- Ankylosis
- Hypofunction of teeth
- Paget’s disease
3. Papillon Lefevre Syndrome
- Juvenile periodontitis
- Palmar plantar keratosis
- Calcification of falx cerebri
4. Desquamative Gingivitis Represents Oral Manifestations Of
- Lichen planus
- Cicatricial pemphigoid
- Pemphigus
Oral Medicine Periodontal Disease Long Essays
Question 1. Describe clinical features, differential diagnosis, and treatment of acute necrotizing ulcerative gingivitis.
Answer:
Acute Necrotising Ulcerative Gingivitis
- Acute Necrotising Ulcerative Gingivitis is a relatively rare condition and is characterized clinically by necrosis of the free gingival margin the crest of the gingiva and the interdental papillae
Acute Necrotising Ulcerative Gingivitis Clinical Features:
- Age – 15-35 years
- Sex – Common in males
- Initially, the gingiva becomes red and painful
- Further, punched-out erosion of the interdental papillae occurs
- Gingiva is covered by a “pseudo-membrane”
- Bleeding occurs spontaneously or on slight provocation
- It produces an extremely unpleasant odor
- The gingival lesion may extend to the mucosal surfaces of the soft palate and tonsils
- It leads to difficulty in deglutition, mastication
- Increased salivation and a metallic taste in the mouth
Read And Learn More: Oral Medicine Question and Answers
Acute Necrotising Ulcerative Gingivitis Generalized Symptoms:
- Headache
- Fever, malaise
- Lymphadenopathy
- Leukocytosis
- Tachycardia
- Gastrointestinal disturbances
Acute Necrotising Ulcerative Gingivitis Differential Diagnosis:
- Primary acute herpetic gingivostomatitis
- Occurs more frequently in children
- Characterized by vesicular eruption
- Erosive lichen planus
- Drug allergy
Acute Necrotising Ulcerative Gingivitis Treatments:
- Removal of pseudomembrane by gently swabbing the area with a cotton pellet
- Rinsing the mouth with a glassful of an equal mixture of warm water and 3% hydrogen peroxide
- Twice daily rinse with 0.12% chlorhexidine
- Antibiotics:
- Penicillin V – 250-500 mg or erythromycin 250-500 mg 6 hourly for 7 days
- Metronidazole 400 mg 8 hourly for 7 days
- Gingival Curettage: After the active phase of the disease
- Supportive Treatment:
- Fluid consumption
- Administration of nutritional supplements
- Antibiotics:
Oral Medicine Periodontal Disease Short Essays
Question 1. Pericoronitis.
Answer:
Pericoronitis
- Pericoronitis refers to inflammation of the gingiva about the crown of an incompletely erupted tooth
Pericoronitis Types:
- Acute
- Sub-acute
- Chronic
Pericoronitis Clinical Features:
- Pericoronitis occurs most often in the mandibular third molar area
- The space between the crown of the tooth and the overlying gingival flap leads to the accumulation of food debris and bacteria
- Thus it is chronically inflamed and infected
- Various degrees of ulceration occurs
- The lesion is red, swollen, and suppurating
- Pericoronitis is tender on palpation
- The pain radiates to the ear, throat, and floor of the mouth
- Presence of foul taste
- Inability to close the jaws
- Swelling of the cheek in the region of the angle of the jaw
- Lymphadenitis
- Fever, leukocytosis, and malaise occur
Pericoronitis Treatment:
- Antibiotics
- Phenoxymethyl penicillin 250 mg 4 times daily
- Metronidazole 200 mg 3 times daily for 7 days
- Drainage
- To allow evacuation of pus
- Extraction – during the sub-acute phase
- Operculectomy – If retention of 3rd molar is preferred
- Extraction of maxillary 3rd molar – when mandibular 3rd molar fully erupts
Question 2. Gingival Enlargement.
Answer:
Gingival Enlargement
- An increase in the size of the gingiva is termed gingival enlargement
Gingival Enlargement Types:
1. Inflammatory Enlargement:
- Chronic:
- It originates as a slight ballooning of the interdental papilla and marginal gingiva
- In early stages, it produces a life-preserver-shaped bulge around the involved teeth
- This bulge can increase in size until it covers part of the crown
- It can be localized or generalized
- Acute Inflammatory Enlargement:
- Gingival Abscess:
- It is a localized, painful, rapidly expanding lesion that is usually of sudden onset
- It is generally limited to the marginal gingiva or interdental papilla
- Initially, it appears as a red swelling with a smooth, shiny surface
- Within 24-48 hours the lesion usually becomes fluctuant and pointed with a surface orifice from which purulent exudates may be expressed
- Periodontal Abscess: It produces enlargement of the gingiva along with the supporting periodontal tissues
- Gingival Abscess:
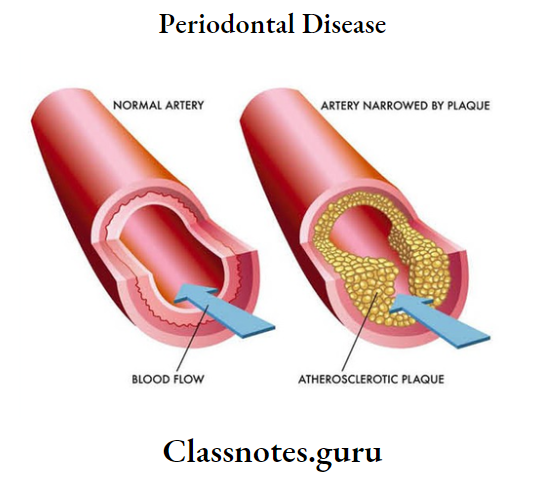

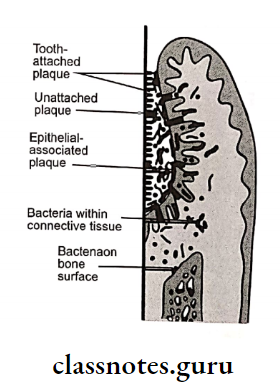
2. Drug-Induced Enlargement: Characterized by bead-like enlargement of the interdental papilla and extends to the facial and lingual gingival margins
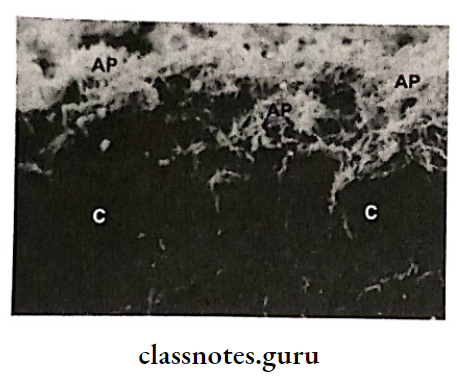
3. Enlargements Associated With Systemic Diseases:
- Conditioned Enlargement:
- Conditioned Enlargement Types:
- Hormonal (Pregnancy, Puberty)
- Nutritional (Vit. C deficiency)
- Allergy
- Conditioned Enlargement Features:
- Gingival edema
- Increased inflammatory response to dental plaque
- Gingiva is bright red/magenta in color
- It is soft and friable
- It has a smooth, shiny surface
- Bleeding occurs spontaneously or on slight provocation
- The lesion appears as a discrete, mushroom-like, flattened spherical mass that protrudes from the gingival margin
- Conditioned Enlargement Types:
- Enlargement Associated With The Systemic Disease: An existing inflammation initiated by dental plaque
4. Neoplastic Enlargement:
- Benign Tumor Of Gingiva:
- Fibroma
- Papilloma
- Leukoplakia
- Malignant Tumor Of Gingiva:
- Carcinoma
- Malignant melanoma

5. False Enlargement: They may appear as a result of an increase in the size of the underlying osseous or dental tissues
Question 3. Halitosis.
Answer:
Halitosis
- Halitosis is an unpleasant odor exhaled in breathing
Halitosis Classification:
- Physiologic halitosis
- Pathologic halitosis
- Pseudo halitosis
Halitosis Causes:
- Physiologic
- Mouth breathing
- Medications
- Aging
- Fasting, starvation
- Tobacco
- Food
- Pathology:
- Periodontal infection
- Tongue coating
- Stomatitis
- Faulty restoration
- Unclean dentures
- Pathologic lesions
- Abscess
Halitosis Diagnosis:
- Subjective Organoleptic Method: It is used as a benchmark
- Gas Chromatography: Measure molecular levels of volatile sulfur compounds
- Halimeters: Measure the level of sulfide gas
- BANA test:
Halitosis Treatment:
- Improvement of oral hygiene and periodontal health
- Tongue brushing should be advised
- Rinsing or gargling with an effective mouthwash
- Halita – It reduces volatile sulfur compound levels
Question 4. Investigation and management of Primary Herpetic Gingivostomatitis.
Answer:
Primary Herpetic Gingivostomatitis Investigations:
- Patient history
- Clinical findings
- Direct smear
- The material is obtained from the base of the lesion and smeared and stained
- The finding of multinucleated cells with swelling, ballooning, and degeneration is adequate for the diagnosis
- Inoculation of the virus from a suspected site to tissue culture
- Serological studies
Primary Herpetic Gingivostomatitis Management:
- Local Applications:
- Using 8% zinc chloride, Talbot’s iodine, phenol, riboflavin, thiamine, etc.
- Chlortetracycline is used as a mouthwash.
- Palliative Treatment:
- Plaque, food debris, and superficial calculus are removed
- Relief in pain is obtained with dyclonine hydrochloride
- Supportive Treatment: Copious fluid intake and systemic antibiotic therapy i.e. aspirin is administered
Oral Medicine Periodontal Disease Short Answers
Question 1. Name drugs causing gingival enlargement.
Answer:
Drugs Causing Gingival Enlargement
- Nifedipine
- Cyclosporine
- Dilantin sodium
Question 2. Epulis.
Answer:
Epulis
- Epulis refers to solid swelling situated on the gum
Epulis Types:
1. Granulomatous Epulis:
- Precipitating factors
- Caries tooth
- Denture
- Poor oral hygiene
- It manifests as a mass of granulation tissue around the teeth on the gums
- It is a soft to firm fleshy mass and bleeds on touch
2. Fibrous Epulis:
- Fibrous Epulis is the most common form
- Fibrous Epulis arises from the periodontal membrane
- Fibrous Epulis is present on the gum
- Fibrous Epulis may undergo a sarcomatous change
- Fibrous Epulis is a firm polypoidal mass, slow-growing, and non-tender
3. Giant Cell Epulis:
- Giant Cell Epulis is an osteoclastoma arising in the jaw
- Giant Cell Epulis presents as hyperemic vascular oedematous, soft to firm gums with indurated underlying mass due to expansion of the bone
- Giant Cell Epulis may ulcerate and result in hemorrhage
- X-ray shows bone destruction with ridging of walls
4. Carcinomatous Epulis:
- This is an epithelioma arising from the mucous membrane of the alveolar margin
- Typically, it presents as a non-healing, painful ulcer
- It slowly infiltrates the bone
Question 4. Drug-induced gingival enlargement
Answer:
Drugs Causing Gingival Enlargement:
Gingival Enlargement Clinical Features
- It occurs 3 months after initiation of phenytoin therapy
- Common in younger individuals
- Generalized distribution but severe in the maxilla
- The site involved- marginal gingiva and interdental papilla
- Appears as a painless, bead-like enlargement
- Interferes with occlusion
- Has lobulated surface
- Firm to resilient in consistency
- No tendency to bleed
Oral Medicine Periodontal Disease Viva Voce
- Drug-inducing gingivitis – phenytoin, cyclosporine, and nifedipine
- Phenytoin-induced gingivitis starts in interdental papillae
- Herpetic gingivostomatitis usually occurs in children and young adults
- Pseudomembrane formation occurs in ANUG
