Local Anaesthesia Important Notes
Local Anaesthesia Classification:
1. Based on the Site of Action:
- Class A: Agents acting on the Exampleternal surface of the membrane: Example- Biotoxins
- Class B: Agents acting on the internal surface of the membrane. Example- Quaternary ammonium compounds
- Class C- Agents acting by independent mechanism- Example- Benzocaine
- Class D- Agents acting by combination mechanisms- Example- Articaine, Bupivacaine
Read And Learn More: Pharmacology Question and Answers
2. Based On Group of Drugs:
- ESTERS
Esters of Benzoic Acids:
- Butacaine
- Cocaine
- HExampleylcaine
- Tetracaine
Esters of Paraamino Acids:
Local anaesthesia questions and answers
B Pharmacy Important Questions
- Chloroquine
- Procaine
- AMIDES
- Atricaine
- Bupivacaine
- Etidocaine
- Quinolone- Centbucridine
Local Anaesthesia Parts:
- Aromatic lipophilic group
- Hydrophilic amino group
- An intermediate chain
Local Anaesthesia Biotransformation:
- Ester group – hydrolysis by plasma cholinesterases
- Amide group – hydrolysis and hydroxylation by microsomal enzymes of the liver
Local Anaesthesia Safe dose:
- A safe dose of 2% lignocaine is
- 4.5 mg/kg or 300 mg without vasoconstrictor
- 7 mg/kg or 500 mg with vasoconstrictor
- Safely dose of adrenaline for dental use
- In normal patients – 0.2 mg
- For cardiac patients – 0,04 mg
Safe dose Actions:
B Pharmacy Important Questions
- Anaesthesia of smaller nerve fibres
- Stimulation of CNS
- Produces vasodilatation
- Produces depressant effect on the myocardium
Local Anaesthesia Adverse drug reactions:
- Intolerance
- Cardiovascular depression
- CNS stimulation
- CNS depression
- Malignant hyperpyrExampleia
Local Anaesthesia Uses:
- Surface anaesthesia – for pain due to burns, ulcers and fissures
- Infiltration anaesthesia
- Nerve block anaesthesia
- Spinal anaesthesia
- Systemic use for anti-arrhythmic effect
Local anesthesia MCQs with answers
B Pharmacy Important Questions Local Anaesthesia Long Essays
Question 1. Classify local anaesthetics and write in detail about xylocaine/lignocaine.
Answer:
Local Anaesthetics:
Local anaesthetics are drugs which cause a reversible loss of sensation in the restricted area of the body either by depression in the Excitation of conducting nerves or suppression of Examplecitation of peripheral nerves.
Local Anaesthetics Classification:
1. Based on chemical structure.
- Amides – Lignocaine, mepivacaine.
- Esters.
- Esters of benzoic acid – Butaaine, cocaine.
- Esters of para-aminobenzoic acid – chloride- caine.
- Quinolones – Centbucridine.
2. Based on the duration of action.
- Injectable anaesthetics.
- Low potency and short duration,
- Procaine, chlorprocain.
- Intermediate potency and duration.
- Lignocaine and prilocaine.
- High potency and long duration.
- Tetracaine, bupivacaine.
- Low potency and short duration,
- Surface anaesthetic.
- Soluble – cocaine, lignocaine, tetracaine.
- Insoluble – benzocaine, tetracaine.
3. Based on biological site and mode of action.
- Class A
- Agents acting at receptor site on Exampleternal surface of nerve membrane.
- Example: biotoxin.
- Agents acting at receptor site on Exampleternal surface of nerve membrane.
- Class B.
- Agents act at receptor sites on the internal surface of the nerve membrane.
- Example: quaternary ammonium compounds.
- Agents act at receptor sites on the internal surface of the nerve membrane.
- Class C.
- Agents act by a receptor-independent physical-chemical mechanism.
- Example: Benzocaine.
- Agents act by a receptor-independent physical-chemical mechanism.
- Class D.
- Agents act by a combination of receptor and receptor-independent mechanisms.
- Examples: Atricaine, lidocaine, mepivacaine.
- Agents act by a combination of receptor and receptor-independent mechanisms.
B Pharmacy Important Questions Local Anaesthetics Mechanism of Action:
Displacement of calcium ions from sodium channel receptor site which permits.
↓
The binding of the LA molecule to this site produces.
↓
Blockade of the sodium channel and decrease in sodium conductance.
↓
Leads to depression in the rate of electrical depolarization.
↓
Failure to achieve the threshold potential level along with.
↓
Lack of development of propagated action potential called.
↓
Conduction Blockade
Xylocaine/Llgnocaine:
- It is the most widely used local anaesthesia.
- It is fast and long-lasting.
- It blocks nerve conduction within 3 min.
B Pharmacy Important Questions Xylocaine/Llgnocaine Actions:
1. Local actions:
- Blocks sensory nerve endings, nerve trunk, neuromuscular junction, ganglionic synapse and receptors.
- Reduces the release of acetylcholine.
- Causes anaesthesia of the skin and paralysis of voluntary muscles.
2. Systemic actions.
- CNS [Central Nervous System]
- Produces stimulation followed by depression.
- Causes blood-brain barrier (BBB).
- Depresses cortical inhibitory pathway.
- Cardiovascular system (CVS).
- Lignocaine decreases Examplecitability, conduction rate and force of contraction.
- Causes hypotension due to vasodilatation and myocardial depression.
- Smooth muscles
- Depresses contraction of intact bowel.
Xylocaine/Llgnocaine Uses:
1. Anaesthesia.
- Used in all types of anaesthesia.
2. Anti-arrhythmia.
Xylocaine/Llgnocaine Adverse Effects:
1. CNS effects.
- Drowsiness, mental clouding, altered tastes, tinnitus.
2. CVS effects.
- Hypotension, bradycardia, cardiac arrhythmia, vascular collapse.
3. Overdose.
- Causes muscle twitching, convulsions, and cardiac arrhythmia.
4. Injections are painful and may delay wound healing.
BDS local anesthesia important questions
Question 2. Mention the types of local anaesthetics.
Answer:
Types of Methods of Local Anaesthesia:
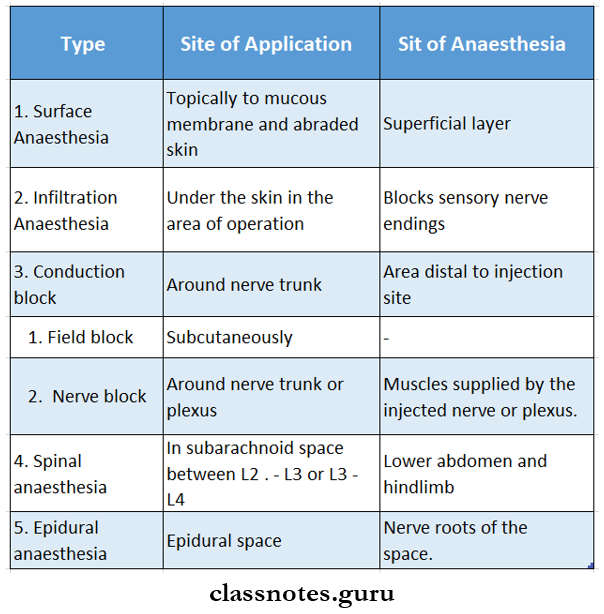
Question 3. Classify local anaesthetics. Compare lignocaine and cocaine.
Answer:
local anaesthetics Classification:
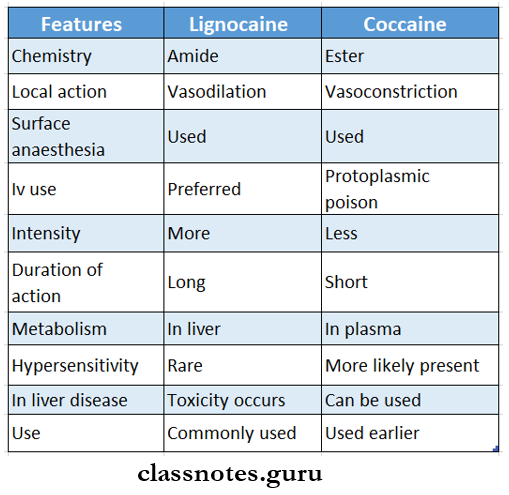
Question 4. Explain how the action of lignocaine can be prolonged.
Answer:
Prolonging Action of Lignocaine:
- The action of lignocaine can be prolonged by the addition of adrenaline.
- Adrenaline reduces the rate of absorption of lignocaine from the site to systemic circulation.
- This prolongs the duration of the action.
- It also reduces the systemic toxicity of lignocaine because of its slow absorption.
- As it gets absorbed, it is metabolized.
Question 5. Write a note on the advantages of lignocaine.
Answer:
lignocaine Advantages:
- Most widely used.
- Versatile, used for all types of blocks.
- Fast and long-lasting.
- Blocks nerve conduction within 3 min.
- More intense.
- Its effect last for 30 – 45 min.
- Available in various forms like spray, gel ointment, and injection.
- Cross sensitivity is not seen with it
B Pharmacy Important Questions Local Anaesthesia Short Essays
Question 1. Uses of adrenaline with lignocaine.
(or)
The rationale of combining adrenaline with Lignocaine.
Answer:
Combining adrenaline with lignocaine has some advantages as well as disadvantages.
Lignocaine Advantages:
- Decreases rate of absorption of lignocaine.
- This prolongs its duration of action.
- Reduces systemic toxicity.
- Increases intensity of nerve block.
- Provides a bloodless field for surgery.
Lignocaine Disadvantages:
- Intense vasospasm and ischaemia in the tissues with end arteries cause gangrene.
- Absorption of adrenaline may cause systemic toxicity.
- It may delay wound healing.
Lignocaine Contraindications:
- The adrenaline + lignocaine combination is contraindicated in
- Cardiovascular disorders.
- Hypertension.
- Congestive cardiac failure.
- Ischaemic heart disease.
Classification of local anesthetics questions
Question 2. Differentiate between general anaesthesia and local anaesthesia.
Answer:
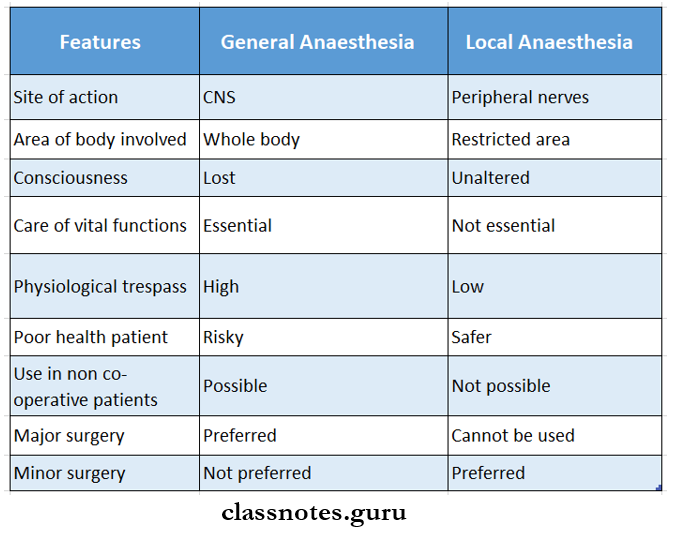
Question 3. Techniques of local anaesthesia with examples
Answer:
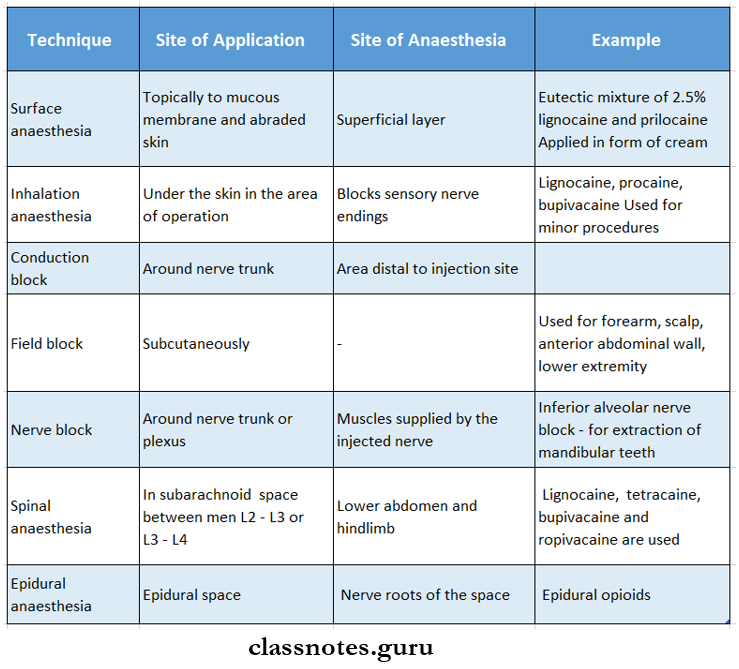
B Pharmacy Important Questions Local Anaesthesia Short Answers
Question 1. Lidocaine/Lignocaine/xylocain.
Answer:
Lidocaine is a long-lasting amide local anaesthetic agent.
- Lidocaine is the most widely used local anaesthetic.
- Lidocaine causes vasodilation in the area of injection.
- Lidocaine is used in all types of blocks.
- Lidocaine is available in various forms.
- Lidocaine effects occur within 3 min and last for 30 – 45 min.
- Lidocaine action can be prolonged by the addition of adrenaline.
- Lidocaine is metabolized in the liver.
- Lidocaine is used in 0.5 – 2% concentration.
Pharmacology of local anesthesia questions
Question 2. Cocaine.
Answer:
Cocaine is a natural alkaloid obtained from leaves of Erythroxylon coca.
- Cocaine is an ester local anaesthetic agent.
- Earlier it was used for ocular anaesthesia.
- Cocaine is well observed.
- As Cocaine is a protoplasmic poison, it is never injected.
- In the periphery, it blocks noradrenaline and adrenaline into adrenergic nerve endings.
- Cocaine causes.
- Local vasoconstriction.
- Tachycardia.
- Rise in BP.
- Mydriasis.
Question 3. Procaine.
Answer:
It is an ester local anaesthetic agent.
- It is the first synthetic local anaesthetic.
- It is metabolized in plasma.
- It is not surface anaesthetic.
Procaine Mechanism:
Hydrolysis of procaine.
↓
Release of para-aminobenzoic acid (PABA)
↓
This antagonises the antibacterial action of sulphonamide.
Question 4. Topical local anaesthetics.
Answer:
- Also known as surface anaesthetics.
- They are available as solutions, ointments, gels, creams, sprays, lozenges, etc.
Topical local anaesthetics Drugs used:
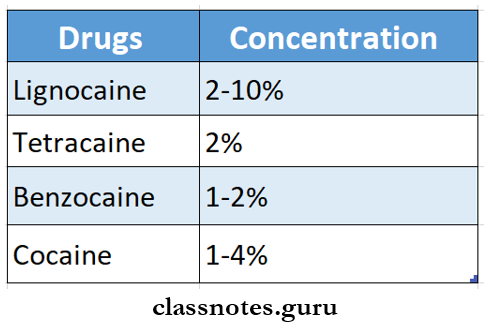
Topical local anaesthetics Uses:
- Applied topically on the mucous membrane of the nose, mouth, eyes, throat, upper respiratory tract, oesophagus, and urethra.
- During endoscopy
- In tonometry of eye.
Local anesthesia viva questions with answers
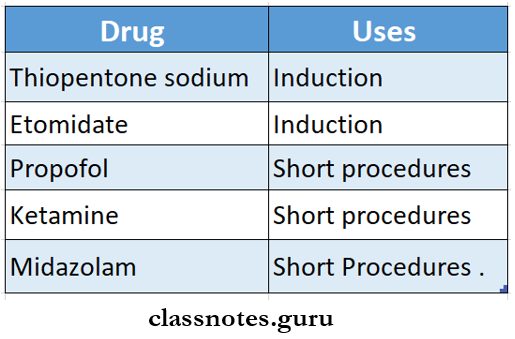
Question 5. Intravenous anaesthesia.
Answer:
Also known as Bier’s block.
- It allows an extremely rapid induction.
- There is no route of quick elimination like lungs for it
- Thus it is used for induction.
- During it, anaesthesia is maintained by an inhalational agent
Dental local anesthesia Q&A
Question 6. Lidocain and mepivacaine.
Answer: